Smart and precise medicine to the aid of lung cancer patients
Editor's note:
Smart medicine is the future of medical advancement. Information technology, artificial intelligence and big data are playing increasingly significant roles in health care, which tends to become more convenient and human-centered. This series on many sectors of the health industry is intended to demonstrate the role of advanced technology, intelligent systems and inventions.
Shot by Jiang Xiaowei. Edited by Sun Chao.
Artificial intelligence and intraoperative pathology are ensuring precise and accurate diagnosis and treatment to patients with lung cancer at the Shanghai Cancer Center, which initiated a new theory of minimally invasive operation imposing the smallest trauma with the biggest benefit to patients.
According to the novel theory, minimally invasive surgery doesn't only mean one or two keyhole cuts but a comprehensive treatment with a small cut, small organ injury and small system injury.
"With the promotion of CT (computed tomography) scans, development of smart medicine and high-quality pathological examination during surgery, we can identify more patients in the early stage and provide most appropriate treatment for smaller post-surgery complications and better life quality. It is the real purpose of early detection and early treatment of lung cancer," said Dr Chen Haiquan, director of the hospital's thoracic surgery department.
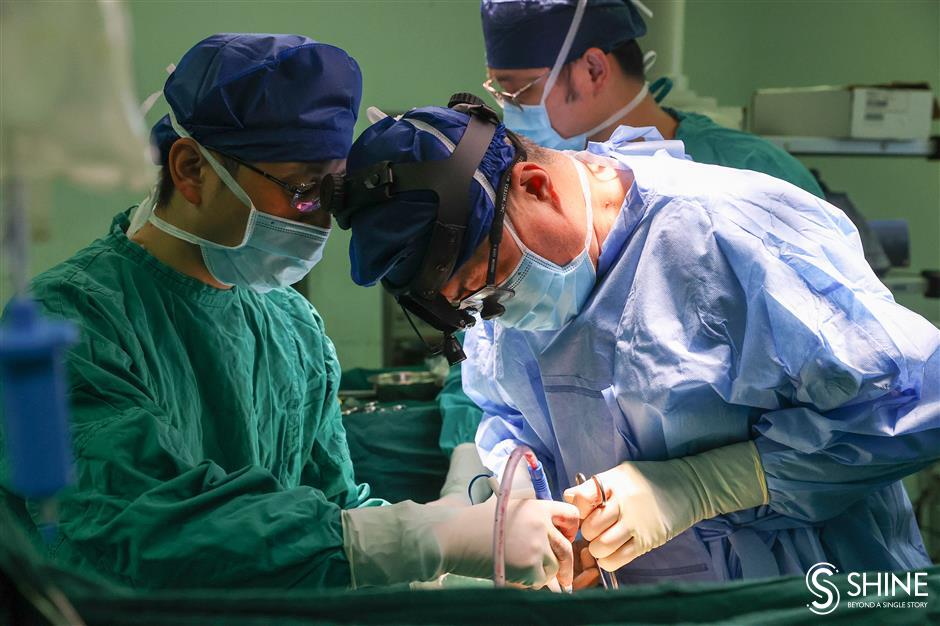
Dr Chen Haiquan (right) conducts a lung cancer surgery.
Lung cancer is one of the most prevalent and deadliest cancers in the world. It is the top cancer in China, which has over 700,000 new cases each year.
"With the rising number of lung cancer patients in the early stage, we are reforming the traditional treatment. Previously, all lung cancer patients had to undergo lung lobe removal and lymphatic node dissection to ensure surgery effects," Chen explained.
"However, our clinical research found that only patients with lymph node metastasis can benefit from the procedure. It can't improve other patients' survival but increases the risk of post-surgery complications, seriously impacting their life quality and recovery.
"Moreover, the lymph node itself is an important immunity tissue. So unnecessary lymph node dissection is not only meaningless but also harmful."

A doctor at the Shanghai Cancer Center processes a sample of lung tissue for intraoperative pathology.

Doctors conduct intraoperative pathology to guide follow-up surgery.
In a bid to identify patients who need the dissection and those who don't, the hospital is one of the first to introduce intraoperative pathology, which means pathologists do timely examination of tissues removed during surgery.
The whole process of intraoperative pathology only takes 20 minutes, said Dr Li Yuan, vice director of the center's pathology department.
Surgeons wait for the result and decide on follow-up procedure. If it's an early-stage tumor and there is no lymph node transfer, they end the surgery. If the pathological test confirms there is a necessity, surgeons expand the surgical scope and conduct the dissection. Each lung cancer patient can receive precise diagnosis and treatment.
Artificial intelligence also supports a precise and efficient diagnosis.

The AI system does a comparison of a patient's lung CT scan.
"Usually, it takes a doctor around 10 minutes to assess a patient's chest CT scans. The doctor needs to evaluate on average around 3,000 images per patient. If it is a complicated case, it can take more time," said Gu Yajia, director of the hospital's radiology department.
"AI just takes seconds. In addition to finding lung nodules, AI can give a primary assessment on the nodules. Doctors will then perform a further and more in-depth evaluation. The process is like a double reading to ensure accuracy.
"AI can greatly reduce doctors' workload and improves efficiency, and is currently most wildly used in lung lesion evaluation."
In addition to diagnosis, AI can accurately compare the sizes of the same lesions from a patient's different assessments, to determine if the lesions were increased in size, or decreased. "If a patient has multiple lesions, it takes a long time for a doctor to do a comparison. It only takes seconds for AI."
AI can also be used for image quality control and to predict therapy efficacy.

The AI system forecasts the result of one treatment.















